- | Corporate Welfare Corporate Welfare
- | Policy Briefs Policy Briefs
- |
First, Do No Harm: Three Ways That Policymakers Can Make It Easier for Healthcare Professionals to Do Their Jobs
COVID-19 presents a challenge of extraordinary scale and complexity. State policymakers across the country, like so many of us, want to know what they can do to help our nation’s healthcare professionals rise to this challenge. Their first task should be to eliminate or suspend laws that stand in the way of patient care. They should consider repealing certificate-of-need laws, eliminating barriers to telemedicine, and liberalizing scope-of-practice rules for healthcare professionals.
Certificate-of-Need Laws
In 35 states and the District of Columbia, certificate-of-need (CON) laws limit the ability of healthcare professionals to open new facilities, expand existing ones, or offer new services. The process covers dozens of technologies and services—everything from drug rehabilitation centers to MRIs. Unlike other types of regulations, the CON process is not intended to evaluate a provider’s competency or safety record. Instead, it is intended to evaluate the provider’s claim that the service is actually needed. Controversially, incumbent providers are invited to challenge the applications of their would-be competitors. Even if a CON is granted, applicants can expect the process to take months or even years, and it has been known to cost providers hundreds of thousands of dollars.
Peer-reviewed academic studies have found that CON laws are associated with higher costs and lower-quality care. But by far the most-studied aspect of CON laws is their effect on access to care. In careful studies that control for possibly confounding effects, researchers find that CON laws are associated with
- fewer hospitals per capita;
- fewer ambulatory surgery centers per capita;
- fewer rural hospitals per capita;
- fewer rural ambulatory surgery centers per capita;
- fewer hospital beds per capita;
- fewer hospice care facilities;
- fewer dialysis clinics;
- fewer hospitals offering MRI, CT, and PET scans;
- longer driving distances to obtain care; and
- greater racial disparities in the provision of care.
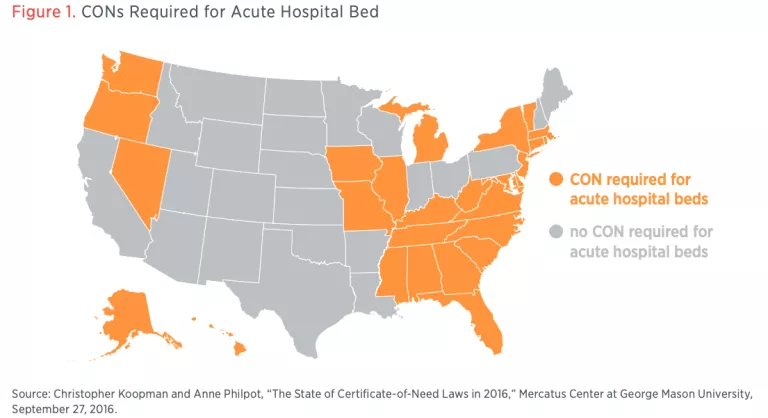
In many cases, the magnitudes of these effects are quite large. The best estimate is that those states that require a CON in order to obtain an acute hospital bed have 1.31 fewer hospital beds per 1,000 residents. To put this in perspective, consider table 1. At 2.77 hospital beds per 1,000 residents, the United States has fewer beds than other countries that have been hard-hit by the coronavirus, including Italy (3.18 beds per 1,000), China (4.34 beds per 1,000) and South Korea (12.27).

Figure 1 shows the 28 states that require providers to obtain a CON before they may acquire an acute hospital bed. In many of these states, hospital systems must obtain a CON even to transfer a bed between facilities.
Healthcare providers in states that eliminated their CON programs years or even decades ago have more beds than non-CON states, are in a better position to quickly obtain new beds, and may quickly reallocate existing ones to the areas where they are needed most.
But it may not be too late for policymakers in CON states. On March 12, the North Carolina Department of Health and Human Services temporarily lifted its requirement that hospitals obtain a CON if they hope to increase their bed capacity by more than 10 percent. And on March 17, Michigan Governor Gretchen Whitmer issued an executive order allowing the Michigan Department of Health and Human Services to issue emergency CONs. Other states are likely to follow suit. South Carolina and Virginia have also suspended portions of their CON process.
Telemedicine
New technologies such as videoconferencing permit healthcare professionals to see and even treat patients from long distances. With overcrowded clinics and hospitals and with health experts exhorting all of us to keep our social distance, telemedicine may be an important front-line tool to diagnose and even treat coronavirus. This is especially true given the rapid pace at which technologies and treatments are advancing. For example, one company claims to have already developed the first at-home coronavirus test.
Federal policy changes surrounding telemedicine are already underway. On March 17, President Trump announced new rules that would permit Medicare to cover telemedical consultations. And the US Department of Health and Human Services recently finalized new rules that would permit physicians who participate in a federal health program to be paid for offering telemedicine services in states where they do not hold a license.
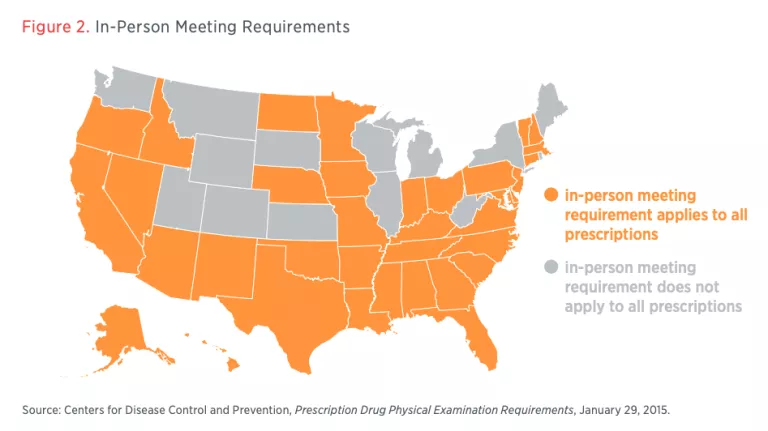
But in many places, state laws may make these federal moves moot. As shown in figure 2, as of 2015, 36 states and the District of Columbia still required an in-person meeting before a provider can write a prescription. In other states, the physical examination requirement only applies to prescriptions for pain-management medications. Moreover, as my colleagues have found, some states require that “an assistant (termed a ‘telepresenter’) be physically present with the patient during a telemedicine encounter.” States may need to relax these rules in order for providers to effectively offer telehealth services during the pandemic.
There is approximately 1 practicing physician for every 500 Americans. But if we include physicians assistants, nurse practitioners, and other highly trained medical professionals, there are about 1.6 medical caregivers for every 500 Americans.
State scope-of-practice laws limit what tasks nurses, nurse practitioners, physicians’ assistants, and other health care providers may do in the course of caring for patients. Two important factors are the degree of autonomous practice and the ability to write prescriptions.
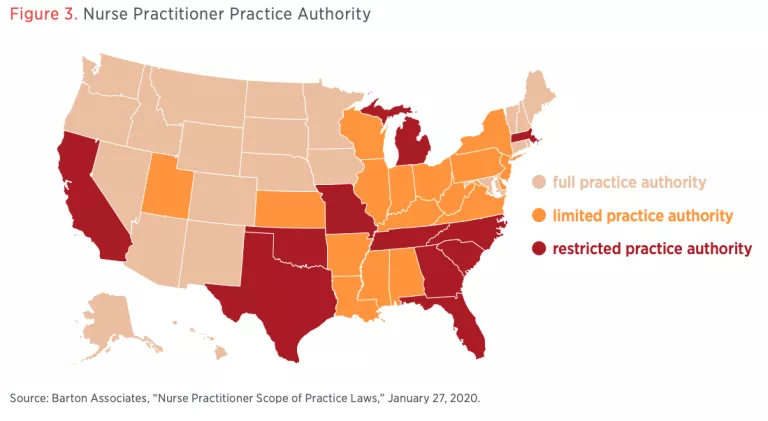
Figure 3 shows how states differ in the degree of autonomous practice authority they permit nurse practitioners. The National Academy of Medicine recommends that nurse practitioners be permitted “full practice authority.” According to the American Association of Nurse Practitioners (AANP), this means that they may “evaluate patients; diagnose, order and interpret diagnostic tests; and initiate and manage treatments, including prescribing medications and controlled substances, under the exclusive licensure authority of the state board of nursing.” Twenty-three states permit this level of authority.
Another 17 states permit a more limited degree of practicing authority. According to the AANP nurse practitioners in these states may “engage in at least one element of NP practice.” Furthermore, in these states, “State law requires a career-long regulated collaborative agreement with another health provider in order for the NP to provide patient care, or it limits the setting of one or more elements of NP practice.”
In the remaining 11 states, nurse practitioners have restricted levels of authority. According to the AANP, this means that “laws restrict the ability of NPs to engage in at least one element of NP practice,” and “state law requires career-long supervision, delegation or team management by another health provider in order for the NP to provide patient care.”
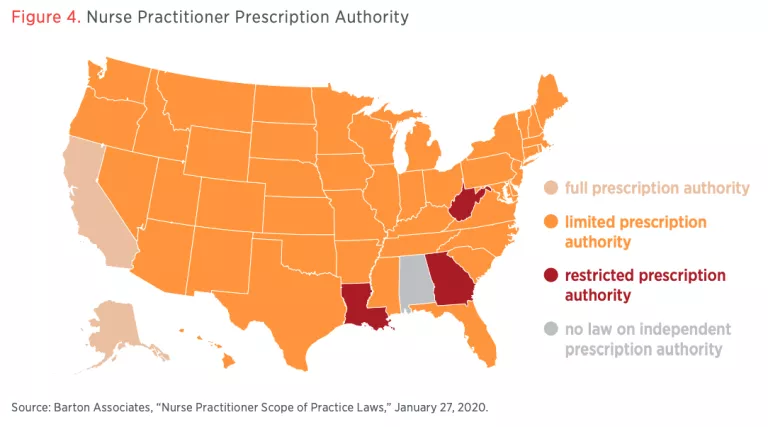
Conclusion
State certificate-of-need laws, restrictions on telemedicine, and scope-of-practice rules should be loosened to allow patients to access care in this time of crisis. Under the best of circumstances, medical professionals should be able to draw on their considerable expertise and training to offer whatever services their patients need whenever and wherever they are located. This is even more important in the midst of a global pandemic.

