For at least 2,500 years, the doctor-patient relationship has resembled the parent-child relationship. The norms of medical ethics, codified in historic documents or perpetuated as informal traditions, encouraged doctors to shield patients from bad news and from general medical knowledge. While Western medical tradition has always included some patient protections, such as informed consent (and its antecedents), doctors have possessed broad powers to withhold treatments that patients desired and, at times, to mislead patients for what they perceived to be the patients’ own good.
The 21st century—and particularly the technological evolution of our era—is dismantling this structure of paternalism. Activities that were once the sole domain of physicians are now conducted by nonphysician professionals (e.g., nurses, pharmacists), by machines (e.g., computers running diagnostic software), and by patients themselves (e.g., using patient-managed diagnostic apps).
The story of medical paternalism’s ascent and decline is described in a new monograph entitled “Anatomy and Atrophy of Medical Paternalism” that I have coauthored with Eric Topol, a preeminent cardiologist and visionary author. I am an economist whose work affords me the pleasure of peering into Topol’s world and offering an outsider’s perspective.
In 21 pages, our monograph travels over a broad sweep of medical history and glimpses a future where the doctor-patient relationship becomes more of a partnership than a guardianship. The parade of characters illustrate the birth, life, and dotage of medical paternalism. The Greek physician Hippocrates advocated and codified paternalized medicine—the notion that the physician is entitled to act as the patient’s agent, and not necessarily with the fully informed consent of the patient. (Some scholars trace this mindset back 4,600 years to Imhotep, an Egyptian who may have been history’s first physician.) The Greco-Roman physician Galen originated at least half a dozen fields of modern medicine; his teachings became unquestioned doctrine to a paternalistic profession up to around the point that certain of his teachings killed George Washington. Benjamin Rush, a signer of the Declaration of Independence, was a great advocate of liberty and equality—except, perhaps, in his sense of entitlement over medical patients. Harvard’s Lawrence Henderson notes that from ancient times till around 1910–1912, physicians almost certainly did more harm than good. Lewis Thomas, dean of medicine at Yale and NYU and president of Sloan-Kettering, described the primitive state (by today’s standards) of medical education at Harvard into the mid-1930s.
“Anatomy and Atrophy” offers an analysis of this parent-child relationship between doctor and patient: why it exists, who enforces it, how it affects health care. The paper also explores the ways in which paternalism is yielding to what Topol has dubbed “the democratization of medicine.”
Our monograph also fits well within the larger body of work from our publisher (and my employer), the Mercatus Center at George Mason University. The passages below will provide a glimpse into “Anatomy and Atrophy” and related pieces published by the Mercatus Center, situating them within the medical environment of 2017.
Decline of Medical Paternalism
Let’s begin this narrative at the end of the “Anatomy and Atrophy” story. After a 2,500-year reign, medical paternalism is giving way to a resurgent democratization. The driving force behind this change is technology. While medical paternalism was never entirely free of controversy, it was, for most of history, relatively easy to justify. Physicians, by dint of education, had knowledge superior to that of their patients. Critical knowledge required years of training and experience, and patients were poorly situated to obtain or process the information. (As the history of Galenism suggests, this medical information was often erroneous—but, nevertheless, it was widely believed and very complex.) In the 19th and 20th centuries, advances in medical science made the doctor’s cognitive advantage far greater.
Now, however, the digital revolution and—ironically—advances in medical science are narrowing the doctor-patient divide. The Internet has placed vast knowledge resources within patients’ reach. Artificial intelligence is reducing broad swaths of medical decision-making to algorithms that allow the disintermediation of certain aspects of medicine. In other words, these technologies allow nonphysician providers (such as nurses), patients, and even intelligent machines to perform functions that once could be performed only by a physician.
But perhaps equally important is the impact of medicine’s most productive century. Up through the mid-20th century, a single physician could grasp a sizable swath of the entirety of medical science. Now, however, medical knowledge has increased so much and so quickly that no individual can grasp more than a small segment of total medical knowledge. Hence, for a specific malady, it is often the case that both patient and physician begin by groping in the dark for information. Hence, patients are no longer in as inferior a position (vis-à-vis doctors) as they were in the past.
Coincident with these developments, recent decades have seen evolution in and strengthening of ethical principles related to the doctor-patient relationship—notably the rules of informed consent.
Motives for Medical Paternalism
In “Anatomy and Atrophy,” we identify three primary motives for medical paternalism. The first is a selective egalitarianism. My recent article speculates on the nature of that egalitarian impulse and how it might impede lifesaving, cost-cutting innovation. The second motive is a selective technophobia—such as the antipathy many doctors demonstrate toward telemedicine, which includes medical examinations conducted through Skype-like cell phone, tablet, or laptop computer interactions. Some states, with the support of the medical community, have inhibited the use of telemedicine, often citing patient welfare as a concern. The third motive is a selective elitism, illustrated starkly by the American Medical Association’s 1847 Code of Medical Ethics, which included the following statement: “The obedience of a patient to the prescriptions of his physician should be prompt and implicit. He should never permit his own crude opinions as to their fitness, to influence his opinions.”
Telemedicine and Selective Technophobia
One of my recent articles contrasts fears of telemedicine with its possibilities, focusing on Doctor on Demand, a prominent telemedicine company with national scope. In 2015, Ian Tong—the company’s chief medical officer—addressed a nationwide conference of state legislators, many of whom were physicians and skeptics about the efficacy of medicine practiced across cyberspace. He related how, in a recent online consultation, he had spoken with a 34-year-old woman who had suffered from nausea, vomiting, and diarrhea for four days but seemed on the mend. Her mother-in-law, unsatisfied, had urged her to contact Doctor on Demand. The screen showed Tong “a young, fit woman with pale lips, speech punctuated by swallows, slow movement for a 34-year-old, pallid lower eyelids and tongue, dry mouth, and poor capillary refill in her fingernail beds.” The mother-in-law measured the patient’s pulse at 108 beats per minute, and the patient reported that standing made her dizzy. Tong correctly surmised that the woman was severely dehydrated or anemic. He sent her to an emergency room for immediate treatment. Had she waited to see her own doctor, as she was inclined to do, she might well have died.
In another article I describe a similar experience with my own mother, whose potentially fatal infection was caught just in time by her grandson, an emergency physician, in the course of a FaceTime conversation via iPad.
Medical Paternalism and the Precautionary Principle
Medical paternalism is related to a broader mindset known as the “precautionary principle.” As described by Adam Thierer, the precautionary principle is “the belief that new innovations should be curtailed or disallowed until their developers can prove that they will not cause any harm to individuals, groups, specific entities, cultural norms, or various existing laws, norms, or traditions.” Thierer contrasts this mindset with its opposite, "permissionless innovation,"
a term he has popularized (particularly in his book Permissionless Innovation: The Continuing Case for Comprehensive Technological Freedom). Thierer describes permissionless innovation as “the notion that experimentation with new technologies and business models should generally be permitted by default.” He elaborates, “Unless a compelling case can be made that a new invention will bring serious harm to society, innovation should be allowed to continue unabated and problems, if any develop, can be addressed later.”
In Thierer’s view, permissionless innovation ought to be the default position, though it should not be an absolute. (Where to draw the line is, of course, the sticky part of such a position.) Permissionless innovation, he argues, is central to a robust environment for innovation. In Thierer’s iconic phraseology, “policymakers should avoid basing policy interventions on hypothetical worst-case scenarios—or else best-case scenarios will never come about.” His advice: “Our policy regime, therefore, should be responsive, not anticipatory.”
Paternalism in the Medical Fortress
My own monograph, “Fortress and Frontier in American Health Care,” explores health care’s philosophical divide between mindsets I refer to as the “Fortress” and the “Frontier”—concepts related to Adam Thierer’s precautionary principle and permissionless innovation. The Fortress is a worldview in two parts: First, public policy’s role in health care ought to be to imagine in advance all the terrible things that might occur in the course of care and to focus resources on prevention of all those untoward events. Second, public policy ought to protect insiders (e.g., doctors, hospitals, drug and device manufacturers, insurers) from upstart competitors. We can think of the Fortress as medical paternalism writ large. In contrast, the Frontier mentality holds that an excessive focus on preventing bad things is undesirable because it stifles the emergence of new modes of treatment that can improve the delivery of care and profoundly reduce its costs. The Frontier view also welcomes the arrival of new competitors to challenge the insiders, both in the provision of familiar forms of care and in new methods of delivery.
For Thierer and for me, the quintessential Frontier industry in the past quarter century has been information technology. Twenty-five years ago, I knew precisely one person who owned a cell phone. It was an unwieldy “bag phone” to use as she traveled between her six or seven homes. In other words, the phone was a symbol of wealth and status. Today, as Eric Topol points out in his book The Patient Will See You Now, there are seven billion cell phones on earth (or SIM cards, at least). Poor developing-country villagers often carry smartphones that, a few decades back, would have ranked among the world’s most powerful computers. All of this was made possible because IT developers did not have to slog through the sort of regulatory processes to which we subject medical innovation; established IT companies obtained no state protection from disruptive competitors. Hence, Apple and Google, founded by uncredentialed developers in garages, rapidly rose to the top of the industry.
Hearing this comparison, some object, saying that health care is different from information technology because it involves life and death, pain and suffering. I generally respond by noting that a technophobe in 1990 could have feared out loud that cell phones and the Internet would unleash death and terror on society: coordinated airliner attacks on buildings, improvised explosive devices, new and large-scale modes of theft and financial chicanery, unprecedented forms of blackmail, instantaneous destruction of reputations, and the ability of anonymous hackers to incapacitate the machines and the institutions that make 21st century civilization possible. The technophobe would have been 100 percent correct. But, even knowing of these horrors, few of us would reverse the IT miracles we’ve witnessed in our lifetimes.
The Pall of Paternalism
“Fortress and Frontier in American Health Care” presents a series of anecdotes that illustrate the benefits of moving beyond the bounds of medical paternalism. My own family doctor in childhood, Milton Ende, was an internist with a superior reputation in our small Virginia town but little profile beyond that. In the early 1960s, he and his brother (a pathologist) began a series of medical experiments in the hospital where I was born. On a therapeutic hunch, the brothers transplanted blood from discarded umbilical cords into the bodies of fully informed terminal cancer patients. These patients showed improvement in their conditions. Though none survived, the experiments suggested the presence of some unknown component in infant blood—a factor that carried some indeterminate healing power.
The Endes, not being part of the academic elite, attracted little attention to their work. Their results were published in an obscure regional journal and then mostly forgotten until, decades later, Scientific American recognized them as pioneers in stem-cell therapy. Their experiment constituted the world’s first cord-blood transplants for cancer therapy. Ultimately, higher-profile researchers conducted parallel research that became mainstream medical science.
While the Endes failed to garner much notice for their work, they could at least conduct their experiments. A half-century later, institutional review boards and other professional norms would probably make such an endeavor impossible. Protecting patients—a worthy goal—has its downside as well.
Drugs and Devices: Faster, Please
One of the great chokepoints in American healthcare innovation is the Food and Drug Administration (FDA). To say this is not to vilify the agency: the origins of the FDA go back over a century, it is staffed by impressive individuals, and it is not difficult to point to major positive accomplishments in the organization’s history. The question is whether its present structure and operating principles have outlived their usefulness.

In a 2015 article called “Replacing the FDA,” I noted longstanding concern over the FDA’s risk-aversion: Milton Friedman, in particular, remarked that the FDA would be vilified if it approved a product that killed 100 people but not if it failed to approve a product that could have saved 100,000. I acknowledge that in the context of the 20th century, the FDA’s mission and structure were defensible. But, we can lay aside the question of whether or not the FDA was an appropriate regulatory vehicle for early- to mid-20th-century conditions. Now, in any case, there is reason to suspect that the FDA’s long, slow, expensive, often-hazy methods for approving new drugs and medical devices may be inadequate for Digital Era innovation.
Richard Williams, Adam Thierer, and I explore this question in depth, arguing that its flavor of medical paternalism “discourages technological innovation and ultimately affects patient choice.” As an alternative model, we suggest examining the European Union’s radically different institutions for approving drugs and medical devices. In the European Union, a set of officially sanctioned private entities (analogous to Underwriters Laboratories) compete to attract prospective drug and device developers. While the FDA suffers few consequences for slow-walking innovation, Europe’s “notified bodies” suffer ill consequences if they either drag out the approval process or recklessly approve dangerous products.
Richard Williams, Marc Joffe, and Ariel Slonim examine the FDA’s role in medical research, particularly singling out cellular therapy, Big Data and the Internet, and synthetic biology. The authors conclude that FDA regulations have impeded scientific breakthroughs, pushing some producers and consumers overseas. One of their examples is the case of 23andMe—the direct-to-consumer genetics test founded and marketed in the United States in 2006 and yanked from the market by the FDA in 2013. In 2017, the FDA approved a highly limited return of the product to the market. (Jordan Reimschisel and I also examine 23andMe in a short piece.)
e-Nable and Democratization of Healthcare Production
“Fortress and Frontier” also discusses an unusual and unusually vivid case of pure permissionless innovation in health care—the e-Nable consortium of volunteers’ production of 3-D-printed prosthetic hands. (I also describe this organization and its prime innovators in a short article.) In South Africa, a carpenter, Richard Van As, accidentally severed several fingers in a table-saw accident. Soon, he contacted Ivan Owen, a puppet-maker in Bellingham, Washington, noted for his intricate mechanical hands. Together, the two worked across a 10,000-mile gap to develop inexpensive but useful and aesthetically pleasing artificial hands. Instantly, the price of a workable hand—good for picking up a coffee cup, riding a bicycle, driving a car, swimming—plunged from around $5,000 (at minimum) to somewhere in the $20–$50 range. For the first time, it became financially practicable to provide working prosthetics for small children, who rapidly outgrow prosthetics.

The Owen–Van As collaboration went viral on the web and spawned a worldwide network of volunteers—often schoolchildren—who manufactured the hands (and arms) and distributed them free of charge. Using open-source software, innovators began modifying the hands to make them more dexterous, utilitarian, and aesthetically pleasing. The desire to connect builders and users grew rapidly, to the point that it became difficult to manage the matchmaking. A technologist and academic, Jon Schull, established a Google Plus group (e-Nable) online to allow individuals to make their own connections, and around the world, thousands of volunteers began producing the hands for thousands of users. e-Nable’s mechanical grasp even extended into war zones, where amputees have proliferated in recent years.
For the most part, the FDA has given e-Nable broad leeway. No FDA approval has been required thus far, but there are bounds on this example of permissionless innovation. If makers began adding motors or sensors to the hands, or if they were to sell them rather than giving them away, it is likely that the FDA would step in and regulate their production and sale. And Owen told me in a conversation that some of the cutting-edge innovation on e-Nable hands is occurring not in the United States but rather in Paraguay, Colombia, and Chile—because their regulators are giving makers wider berth to innovate.
Distribution or Growth? The Calendar Test
Our national healthcare debate has been stuck in the Fortress for many decades. The strong undercurrent of medical paternalism leads us to focus on health insurance rather than on changing the way we actually deliver care. Recently, I offered a thought experiment—the Calendar Test—to illustrate the problem. The Calendar Test imagines a primary care doctor who works ten hours per day. For five hours, he does administrative and educational tasks; for the other five, he sees 20 patients a day for 15 minutes apiece. Now, someone hands out four gift coupons good for one visit to the doctor today. There are four ways the doctor can handle this increase in patient load. The first three mostly redistribute existing resources: (1) Work an extra hour or two. (2) Reduce the time spent with each patient. (3) Kick four current patients off of the calendar. (The Affordable Care Act, I argue, focused on the second and third options, shifting who had priority for appointments and who paid how much for what. And I argue that most GOP alternatives to the ACA do essentially the same thing.)
The fourth option is to actually change the way we deliver health care—to provide more care for less expenditure. For the most part, reforms that pass the test are those that shift the burden of care away from physicians and toward nonphysician providers (e.g., nurse practitioners or pharmacists), machines (e.g., IBM’s Watson computer or more common automated tools), and patients. A strong current of medical paternalism may inhibit all three of these shifts.
Darcy Bryan, a California obstetrician and gynecologist, and I are researching the centrality of electronic health records to freeing up the doctor’s calendar. A brief introduction to this research is found in our article “Toward Digital Health Biographies.”
AliveCor and Me
For personal reasons, I’ve written and spoken repeatedly on one concrete example of shifting the burden of care off the physician’s calendar and onto machines and patients themselves. In 2016, I experienced a brief episode of atrial fibrillation—an arrhythmia of the heart. A-fib, as it’s known for short, can cause debilitating or even lethal strokes if left untreated. After this episode, the cardiologist put me on a beta blocker and at this point I’ve gone over a year without any further episodes.
Ten days or so after the episode, the doctor had me to go for several days without the medication so she could administer a treadmill stress test. One evening during this period, I thought I was having another episode. I returned to the emergency room and was wired up for an electrocardiogram (EKG) and other metrics. The results showed that I was fine. The trip to the emergency room had been unnecessary. Someone paid several thousand dollars in bills for my privilege of being told, “Go home. Nothing wrong.”
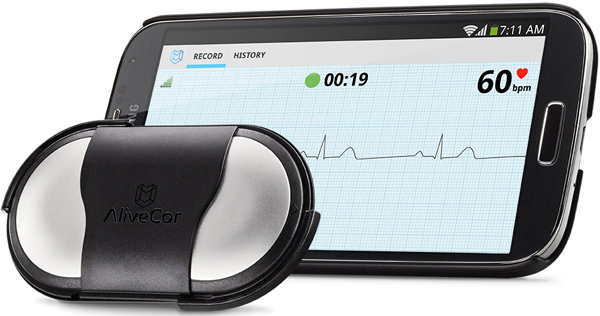
Some weeks later, while driving on a remote road a distance from any towns and perhaps 15–20 miles from the nearest hospital, I thought once again that I was having an episode of A-fib. By now, however, I had bought two devices. One was a Fitbit that showed that, indeed, my pulse was accelerating quite a bit. The second was an AliveCor Kardia—a patient-operated device that fits on the back of my cell phone and allows me to take my own EKG and to receive an instant diagnosis, conducted via artificial intelligence. As I began to think about where I might find a clinic (this was at twilight), I pulled into a service station, took an EKG, and received a clean diagnosis. My heart rate was a little fast, but in normal rhythm. I returned to my car and drove four hours to my home. As I drove, I thought, “America’s healthcare expenditures will be several thousand dollars lower in 2016 because I purchased a $99 smartphone device.”
In the year since, the AliveCor has brought me great peace of mind. The device is FDA-approved and yields clinical-quality EKGs. Still, some physicians are deeply skeptical about relinquishing this role to patients. On at least one occasion, a physician seemed agitated by my use of such a device and expressed a strong preference for a face-to-face doctor-patient relationship. I responded by noting that despite the excellent relationship I have with my doctor, she was not going to make an appearance on a desolate road, four hours from home, as the sun was setting.
Curiously, my episode of atrial fibrillation came less than 24 hours after I had delivered a lecture on AliveCor, which I had learned about by reading Eric Topol’s The Patient Will See You Now.
Healthcare Openness and Access Project (HOAP)
Those of us who follow healthcare policy for a living tend to think first and foremost about the federal government. But in the United States, states have enormous, if underappreciated, control over the delivery of care. In 2016, Darcy Bryan, Jared Rhoads, and I developed the Mercatus Center’s Healthcare Openness and Access Project (HOAP). HOAP looks at 38 separate variables measuring the discretion patients and providers have over broad areas of health care. These variables are grouped into broad indexes indicating the flexibility of state laws and regulations concerning telemedicine, medical liability, health insurance, and so forth.
Certificate of Need Requirements
One of the variables measured by HOAP is the presence or absence of certificate of need (CON) legislation.
CON laws require hospitals (and sometimes other healthcare providers) to get permission from the state before making changes such as opening a new facility, adding patient capacity, or even purchasing individual pieces of equipment. Matthew Mitchell and Christopher Koopman have explored the history and economic impact of such laws. Mitchell looks at the original motives behind CON requirements and asks whether those goals have actually been met. A sizable number of Mercatus papers look at issues related to CON; for instance, Thomas Stratmann and David Wille look at the impact of such laws and conclude, “Our overall results suggest that CON regulations lead to lower-quality care for some measures of quality and have little or no effect on other measures of quality.”
While analysis of CON tends to focus on cold numbers, such as the number of CON laws and regulations in effect in various states, it is vital to remember that CON requirements can have a deep human impact. For example, a hospital near Roanoke, Virginia, had sought for years to use its own money to purchase equipment for distressed newborns. For years, the state’s CON laws (in Virginia called the certificate of public need program) had prevented the purchase from occurring. In one case reported in the press, a distressed newborn arrived at the hospital but was sent to a neighboring town whose hospital had the necessary equipment. The infant died en route to the other hospital.
Herodotus and Nightscout
What is old can become new. “Anatomy and Atrophy” begins with an observation by the Greek historian Herodotus around 400 BCE. The Mesopotamians, he noted, had no physicians. Sick patients were taken to the town’s central marketplace, where passersby were asked whether they had seen similar cases and, if they had, were asked to offer their suggestions for treatment. Two and a half millennia later, the Internet has reinvented this mode of care: now it is known as crowdsourcing. “Anatomy and Atrophy” recounts the story of an old friend of mine, Arturo Porzecanski, who suffers from systemic capillary leak syndrome, a rare and potentially deadly condition most physicians have never seen. The web brings together patients and doctors from around the world to share observations and ideas about this rare condition—it is an updated version of the Mesopotamian marketplace.
Increasingly, too, modern social media have become a venue for the invention of new modalities of treatment. One of my articles describes Nightscout—a group of high-level computer programmers with diabetic children. They have turned cell phones into remote-monitoring devices for their children’s insulin pumps. To plunge ahead, they have skated around the outer limits of FDA approval. Their motto, which we might view as a direct assault on medical paternalism, is encapsulated in their hashtag: #WeAreNotWaiting.
The Promise of a More Open Future
There is very little in society that has survived the last 2,500 years without great changes, and there is no reason to think that the practice of medicine should be any different. While never perfect, medical practitioners have always attempted to build institutions that lead to the best outcomes. The paternalistic structure was long viewed as the best foundation for medical treatment because it provided value and arguably did a better job than other available options. In many ways, the ground is shifting under that assumption.
As so many examples in other aspects of our lives have proved, we should embrace the pioneering, entrepreneurial, and innovative behaviors that have advanced and improved all of our lives. Of course, caution is advisable, but not to the point of paralysis. Will we pledge continued policy deference to the Fortress that increasingly obstructs real progress in medical care? Or will we embrace the Frontier and promote the innovation that has benefitted us in so many other parts of our lives?