- | Healthcare Healthcare
- | Research Papers Research Papers
- |
2016 Edition: Healthcare Openness and Access Project
How accessible is health care in your state?
There is broad agreement in the United States that it would be desirable to lower the cost and improve the quality of health care and broaden health insurance coverage. There is much disagreement about how this trio of goals is to be accomplished. The years-long political struggle over the Affordable Care Act (ACA, commonly known as Obamacare) is the most visible manifestation of this divergence of views. The ACA represents one approach to tackling the three goals. Many on the political Left argue for still-more-centralized public-sector control over health care and particularly for a federal single-payer insurance system. Policymakers and commentators on the Right have offered a variety of proposals that, generally speaking, would shift more power to private-sector entities and to states. All these proposals have one thing in common: they assume the key to lower costs and better care lies in reconfiguring the insurance system.
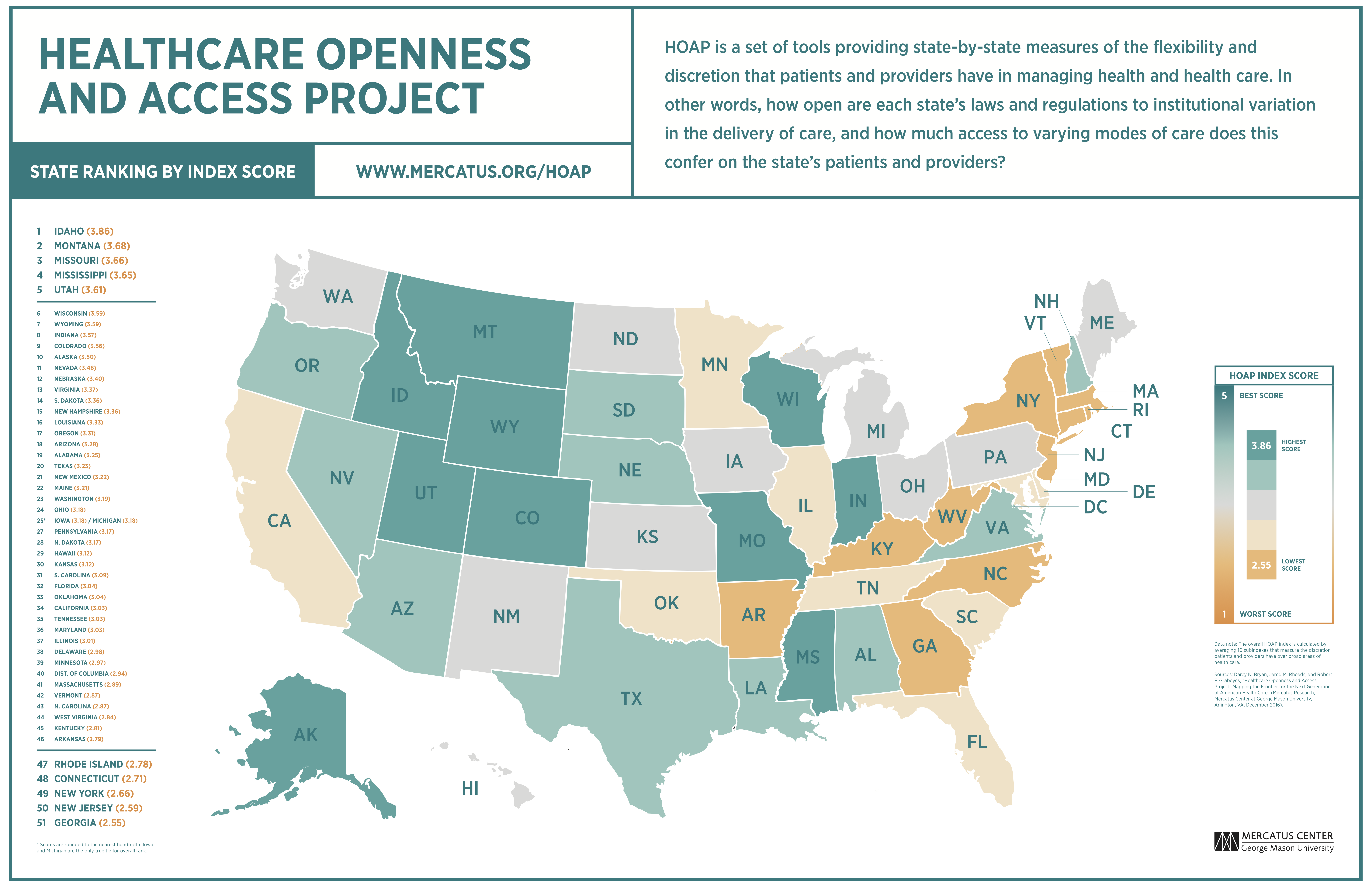
We believe the three goals of healthcare reform cannot be attained by fixating solely, or even primarily, on health insurance reform. States have (and should have) substantial control over the delivery of health care—and not solely or principally in the area of insurance reform. To make maximum use of state powers in improving care, it is vital to have a basis for comparison—to see what works in other states. The Healthcare Openness and Access Project (HOAP) is a set of tools providing state-by-state measures of the flexibility and discretion that patients and providers have in managing health and health care. In other words, how open are each state’s laws and regulations to institutional variation in the delivery of care, and how much access to varying modes of care does this confer on the state’s patients and providers?
Five motivations prompted HOAP’s creation:
- Insurance isn’t everything. Ultimately, simultaneous progress on the three goals of healthcare reform—lower costs, higher quality, and broader coverage—will require fundamental changes in the technologies and structures of care and in how, where, when, and why care is delivered. Those fundamental changes will be most effective, we believe, not as top-down mandates based on centralized expertise, but rather as the results of a vast constellation of patients and providers innovating, experimenting, and extemporizing to an unprecedented degree. HOAP highlights institutional features that help determine the degree to which such experimentation is currently possible.
- States matter. States possess great power to determine which providers perform what services, the means by which they do so, their legal responsibilities in the event that patients suffer harm, and so forth. The HOAP index and subindexes suggest how the states differ in encouraging delivery-system innovation. To be sure, insurance is part of the equation, and HOAP data do include some insurance-related variables.
- Perception is not reality. Perceptions about states do not always accord with reality. A leftward tilt in the ACA debate does not necessarily correlate with tight centralized control of health care at the state level. Nor does a rightward tilt in the debate always comport with extensive patient-provider discretion. For example, HOAP suggests that Oregon, a reliably blue state, offers broad leeway to patients and providers while Georgia, a very red state, has some of the most restrictive healthcare laws and regulations in the nation.
- Comparisons help. HOAP as a whole provides a great deal of comparative data on healthcare policy in the states. It is a one-stop source of information on policy differences around the country. As an example, 48 states and the District of Columbia forbid over-the-counter sales of oral contraceptives. So, to many, that prohibition may seem to be the natural order of things—a universal. But it is not without exception: California and Oregon do allow such sales. Perhaps this anomaly will persuade policymakers in other states to at least ask how that market functions in the two outlier states. Do over-the-counter sales cause prices to drop? Are there measurable effects on health—either positive or negative? How do patients and providers in California and Oregon feel about this example of autonomy?
- Discussion is valuable. We want HOAP to become a catalyst for discussion. We do not present the index as the definitive measure of openness, access, flexibility, or discretion in health care for any particular state. Rather, it is a first pass, an approximation, a point of departure. If observers question aspects of the index and offer alternatives, then the project will have done its job.
In 1883, the great physicist and engineer Lord Kelvin famously stated what has since become known as Lord Kelvin’s dictum: “When you can measure what you are speaking about, and express it in numbers, you know something about it; but when you cannot measure it, when you cannot express it in numbers, your knowledge is of a meagre and unsatisfactory kind; it may be the beginning of knowledge, but you have scarcely, in your thoughts, advanced to the stage of science, whatever the matter may be.”
We offer HOAP in the spirit that Lord Kelvin expressed. At the same time, we humbly keep in mind the addendum offered decades later by the great economist Frank Knight: “And when you can measure, your knowledge is of a meager and unsatisfactory kind.”
Project Design
The overall HOAP index is the average of 10 equally weighted subindexes that measure the discretion patients and providers have over broad areas of health care, such as public health and telemedicine. The equal weighting is purposeful: it is an explicit recognition of the fact that no single set of weights should be considered “correct.” In any project of this type, the menu of component variables is somewhat arbitrary and subjective. We have constructed HOAP so readers and researchers can, if they wish, alter those weights to reflect their own preferences. It would please us to find others using HOAP data to devise alternative indexes whose findings deviate from ours.
The subindexes are, in turn, averages of equally weighted indicators. The Taxation Subindex, for example, is the average of three indicators related to taxes on providers, health savings accounts, and medical devices. The 38 indicators (which are really sub-subindexes) are calculated in a variety of ways from various data sources. Details on data sources and calculations are provided in appendix B of the project overview document.
Here is a list of the subindexes (in alphabetical order) and the indicators that compose the overall HOAP index:
Corporate Subindex
- State allows the corporate practice of medicine
- State allows businesses to employ licensed healthcare professionals
- State allows nonlicensed individuals to own/operate medical entities
- State allows licensed individuals to split fees with nonlicensed individuals
Direct Primary Care Subindex
- State has pro-DPC laws
- State has higher market demand for DPC
- State has more DPC practices per capita
Insurance Subindex
- State mandates fewer health insurance benefits
- State mandates less rate review
- State does not expand on federal age rating limitations
- State does not expand on federal tobacco rating limitations
- State does not expand on federal geographic rating limitations
Medical Liability Subindex
- Physicians pay fewer malpractice actions
- Physicians pay lower malpractice premiums
- State has adopted more reforms to modulate malpractice litigation
Occupational Regulation Subindex
- State allows medical licensure reciprocity with other states
- State has fewer continuing medical education requirements
- State allows nurse practitioners broad scope of practice
- State has fewer optician licensing requirements
- State allows direct-entry midwifery
Pharmaceutical Access Subindex
- State allows greater access to experimental drugs
- State allows access to medical marijuana
- State allows easier access to pseudoephedrine
- State allows over-the-counter access to oral contraceptives
Provider Regulation Subindex
- State has fewer certificate-of-need restrictions
- State puts fewer restrictions on compounding pharmacies
- State lacks burdensome prescription monitoring mandates
Public Health Subindex
- State allows access to e-cigarettes
- State allows access to naloxone
- State has strong “Good Samaritan” protection
Taxation Subindex
- State has fewer provider taxes
- State has fewer health savings account (HSA) taxes
- State has fewer medical device taxes
Telemedicine Subindex
- State reimburses Medicaid providers at parity for telemedicine
- State has less restrictive telepresenter requirements
- State reimburses Medicaid providers at parity for remote monitoring
- State allows online prescribing
Caveats and Conclusions
As we have noted, any index of this type necessarily involves a substantial measure of subjectivity and arbitrariness. There is also a degree of ambiguity. Implicitly, a higher score on the overall index or a particular subindex suggests “better” conditions than a lower score does, but the case for one score being better than the other may not be clear.
For instance, one indicator for the Telemedicine Subindex involves Medicaid reimbursement parity. We take it as beneficial that, in some states, Medicaid will pay for telemedicine. But parity itself is problematic. One argument for telemedicine is that it is less costly than traditional office visits. Therefore, if Medicaid pays the same amount for both, it may be depriving telemedicine practices of the ability to compete on the price dimension—to push costs downward. To offer another example, our index implies that the availability of pseudoephedrine is a positive opportunity for patients who suffer from allergies. We recognize, however, that states make the purchase of these drugs difficult because pseudoephedrine can be used in the production of illegal addictive drugs such as methamphetamine. Hence, we include the pseudoephedrine access indicator with reservations.
We use a 1|2|3|4|5 Likert scale for all indicators. Some indicators, however, are binary. In those cases, we opted to use 1 and 5. We could have chosen, say, 2 and 4, knowing that doing so would reduce these indicators’ impact on subindexes and the overall index. Again, one must choose, and there is no unambiguously correct choice.
While we recognize some haziness in the data, we nevertheless see the results as meaningful information. If one state ranks third and another fourth in the HOAP index, that is rather weak evidence that flexibility is greater in the first state. But if one state ranks third and another ranks forty-seventh, that is more likely to be a meaningful distinction.
We decided to omit certain variables because they are so politically charged that their presence might drown out the overall findings—and because even among the creators of HOAP there are strong differences of opinion on the positives and negatives of these issues. Three that come to mind are abortion, assisted suicide, and vaccination exemptions. They are nowhere to be found in this project.
In some ways, the goal of HOAP is to encourage questions rather than to provide definitive answers. HOAP is a journey, not a destination.