- | Academic & Student Programs Academic & Student Programs
- | Healthcare Healthcare
- | Research Papers Research Papers
- |
2018 Edition: Healthcare Openness and Access Project
Mapping the Frontier for the Next Generation of American Healthcare, June 2018 Update
There is broad agreement in the United States that it would be desirable to lower the cost and improve the quality of healthcare and to broaden health insurance coverage. There is much disagreement about how this trio of goals is to be accomplished. Proposals from various political perspectives have one thing in common: they assume the key to lower costs and better care is to reconfigure the insurance system.
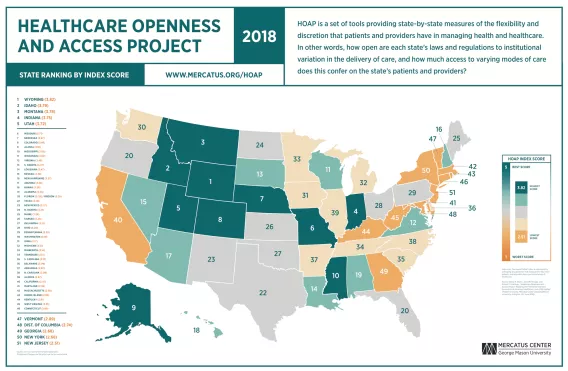
However, health insurance reform should not be the sole fixation of reform efforts. States have (and should have) substantial control over the delivery of healthcare—and not solely or principally in the area of insurance reform. To make maximum use of state powers in improving care, it is vital to see how institutions work in other states. In the Healthcare Openness and Access Project (HOAP), Darcy N. Bryan, Jared M. Rhoads, and Robert F. Graboyes present state-by-state measures of the flexibility and discretion that patients and providers have in managing health and healthcare.
HOAP seeks to raise important questions, such as how open each state’s laws and regulations are to institutional variation in the delivery of care and how much access to varying modes of care this confers on the state’s patients and providers. The goal of HOAP is to encourage these types of questions rather than to provide definitive answers.
Background and Study Design
The years-long political struggle over the Affordable Care Act (ACA) is the most visible manifestation of the divergence of views about how to improve healthcare. The ACA represents one approach to tackling the three goals. Many on the political Left argue for more centralized public-sector control over healthcare and for a federal single-payer insurance system. Others on the political Right have offered a variety of proposals that would shift more power to private-sector entities and to states.
HOAP’s overall index averages 10 equally weighted subindexes that measure the discretion patients and providers have over broad areas of healthcare, such as public health and telemedicine. The equal weighting is an explicit recognition of the fact that no single set of weights should be considered “correct.” HOAP is constructed so that readers and researchers can alter the weights assigned to different variables to reflect their own preferences.
HOAP was originally issued in December 2016. In June 2018, the numbers were revised to reflect changes in state laws in the interim and to reflect modest changes in the HOAP methodology. Changes in state rankings reflect both of these factors, so one should be cautious about reading too much into the numeric differences between the first and second versions of HOAP.
Key Points
- Insurance isn’t the only issue. Ultimately, simultaneous progress on the three goals of healthcare reform—lower costs, higher quality, and broader coverage—will require fundamental changes in the technologies and structures of care and in how, where, when, and why care is delivered. HOAP highlights institutional features that help determine the degree to which experimentation is possible.
- States matter in healthcare policy. States possess great power to determine which providers may perform what services, the means by which they may do so, their legal responsibilities in the event that patients suffer harm, and so forth. The HOAP index and subindexes suggest how the states differ in encouraging delivery-system innovation. To be sure, insurance is part of the equation, and HOAP data do include some insurance-related variables.
- Perception of state policies does not always match reality. Perceptions about states do not always accord with reality. A leftward tilt in the ACA debate does not necessarily correlate with tight centralized control of healthcare at the state level. Nor does a rightward tilt in the debate always comport with extensive patient-provider discretion. For example, HOAP suggests that Hawaii, a reliably blue state, offers considerably broader leeway to patients and providers than does Georgia, a very red state with some of the most restrictive healthcare laws and regulations in the nation.
- Comparisons among states are important. HOAP as a whole provides a great deal of comparative data on healthcare policy in the states. It is a one-stop source of information on policy differences around the country. As an example, 47 states and the District of Columbia require a physician’s signature to prescribe oral contraceptives. While that requirement may seem to be standard, California, Oregon, and Colorado allow pharmacists to autonomously prescribe oral contraceptives. This anomaly may persuade policymakers in the states that do not allow such sales to investigate how the market for oral contraceptives functions in the three outlier states.
- Discussion is valuable to determine how to move forward. HOAP should become a catalyst for discussion, but it is not the definitive measure of openness, access, flexibility, or discretion in healthcare for any particular state. If observers question aspects of the index and offer alternative measures, then the project will have done its job.
To speak with a scholar or learn more on this topic, visit our contact page.


