- | Healthcare Healthcare
- |
Minnesota and Certificate-of-Need Programs 2020
How CON laws Affect Health Care Access, Quality, and Cost in Minnesota
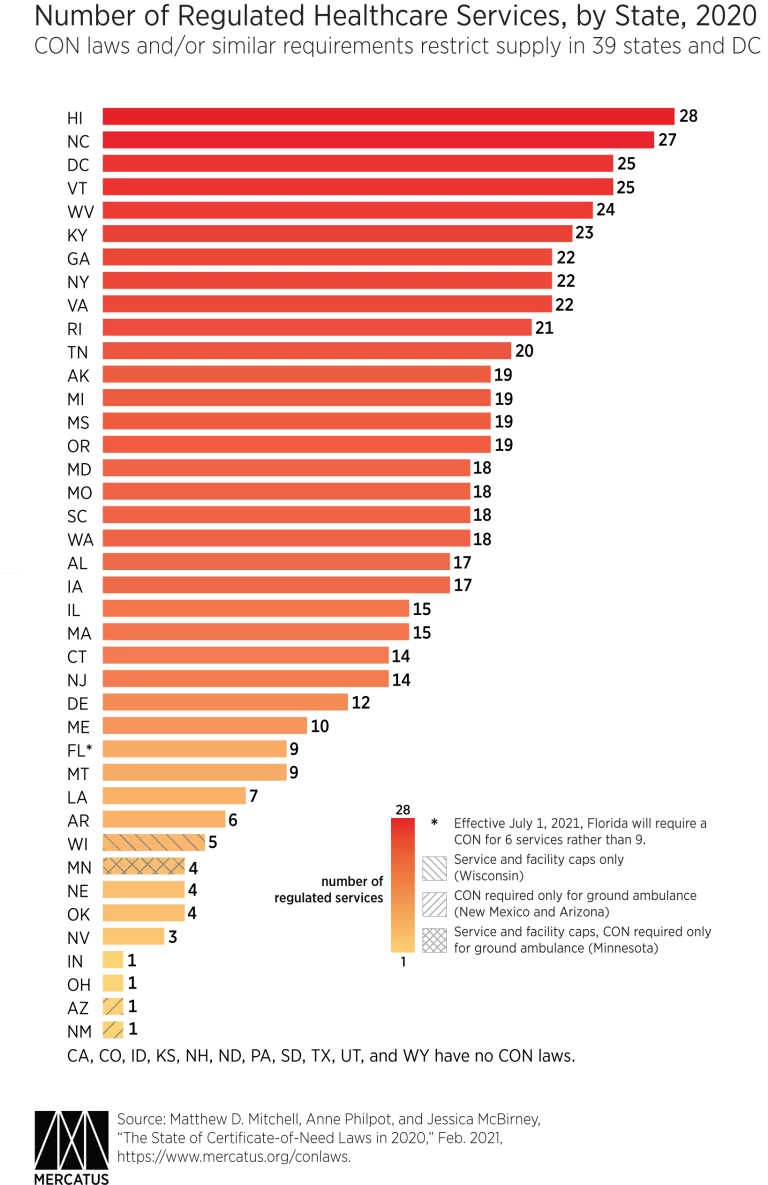
Minnesota regulates ground ambulance services with a certificate-of-need (CON) law. CON laws require healthcare providers to obtain permission before they open or expand their services or purchase certain devices or new technologies. CON applicants must prove that the community needs the new or expanded service, and existing providers are invited to challenge would-be competitors’ applications. CON laws have persisted in spite of mounting evidence from health economists, regulatory economists, and antitrust lawyers showing that these laws fail to achieve their intended goals.
Minnesota also operates a program that is similar to CON regulation, setting numerical caps on three service categories. Once the state reaches these thresholds, providers are not allowed to further increase supply.
This profile highlights the state’s ground ambulance CON and the services that Minnesota caps. Because Minnesota’s CON program is limited to ground ambulance services and because there is less research on caps relative to CON laws, we do not offer any predictions about healthcare cost, quality, or access in the absence of these regulations.
CONs and Caps on Healthcare Services in Minnesota as of January 2020
- CON on Ground Ambulance services
- Cap on Hospital Beds (Acute, General Licensed, Med-Surg, etc.)
- Local CONs on Intermediate Care Facilities (ICFs) for Individuals with Intellectual Disabilities
- Cap on New Hospitals or Hospital-Sized Investments
- Cap on Radiation Therapy
These types of restrictions are in addition to the standard licensing and training requirements for medical professionals, but are neither designed nor intended to ensure public health or ensure that medical professionals have the necessary qualifications to do their jobs. Instead, CON laws are specifically designed to limit the supply of health care and are traditionally justified with the claim that they reduce and control health care costs. The theory is that by restricting market entry and expansion, states will reduce overinvestment in facilities and equipment. In addition, many states—including Minnesota—justify CON programs as a way to cross-subsidize health care for the poor. Under these “charity care” requirements providers that receive a certificate of need are typically required to increase the amount of care they provide to the poor. These programs intend to create quid pro quo arrangements: state governments restrict competition, increasing the cost of health care for some, and in return medical providers use these contrived profits to increase the care they provide to the poor.
How to Reform State CON Laws
Eleven states have already done away with their CON regulations, and many legislators rightly see CON repeal as a common-sense way of improving health care in their states. While full repeal is best, there are still ways to make meaningful reforms happen even when full repeal is not feasible.
Explore Options for Reforming CON Laws
.fsSubmitButton {line-height:0 !important; height:58px !important; font-size: 16px !important; font-family: Gotham A,Gotham B !important; padding: 20px !important; width:100%;} button .fsNextButton {line-height:0 !important; font-size: 16px !important; font-family: Gotham A,Gotham B !important; padding: 20px !important;} .fsSubmit, .fsForm {padding:0 !important;} .fsPage, .fsForm, .fsSingleColumn {background-color:#EAEAEA !important;} .fsBody{padding:0 !important}
